Perimenopause - a definition
Perimenopause is not just 'the time before menopause'. It is defined by clinical standards laid out by a framework called STRAW.

The ovarian aging naming system
Symptoms of ovarian aging can happen long before the final menstrual period (FMP).
Most public narratives would refer to this time as 'perimenopause'. However, this can create challenges for this seeking guidance and support from their doctors.
The clinical framework works - if we all use it.
When talking to groups, social media-ing or blogging about anything to do with menstrual health we need to make sure we are being 'safe, sensible and supportive'. It's very easy to get carried away in the narrative - been there, done that!@everyone
I too would have said, 'perimenopause starts years before menopause day', in order to make the point that signs, indicators and symptoms are appearing way before you think. It's an easy mistake to make unless you top and tail the sentence.
Try this checklist of what's happening in the sequence to make sure you are in the safe arena when sharing information:
Signs and indicators of change in ovarian activity happen a lot earlier than you realise ---> potentially from the tipping point (TP) forward, which is NOT perimenopause. This is called late reproductive.
For non Menopause School students, the tipping point is when the ovaries have an egg reserve of ~25K, typically around the age of 37.5. After this point ovarian aging begins to accelerate in an irregular way. Prior to this point it was fairly constant. You can read more here
The signs and indicators of changes in physical and emotional characteristics, after TP, are unlikely to be noticed by an individual - unless they are very connected to their own self, and/or tracking + journaling their menstrual cycle.
Remember at this point there is no noticeable change externally in the cycle, but there will be internally. Or as STRAW say, 'critical endocrine parameters begin to change before overt changes in menstrual cyclicity'.
The signs and indicators probably go unnoticed, or unconnected to ovarian aging, until they become more noticeable, and then will mostly be described as 'symptoms'. There may still be no noticeable change externally in the cycle but ovarian activity/aging is happening.
The definition of early perimenopause = a change in 7 days between cycles, and late perimenopause includes episodes of no bleeding for 60+ days
NO clinical, researched guidance talks about levels of hormones in terms of symptoms, at any point. We subscribe to the principles of #VerifyBeforeYouAmplify which makes us 'safe, sensible and supportive'
Symptoms of ovarian aging along the timeline are caused by sensitivity to changes in hormone signalling not absolute levels as published by SWAN in 2012 and review here by the AHA in 2023 https://www.ahajournals.org/doi/full/10.1161/CIR.0000000000000912
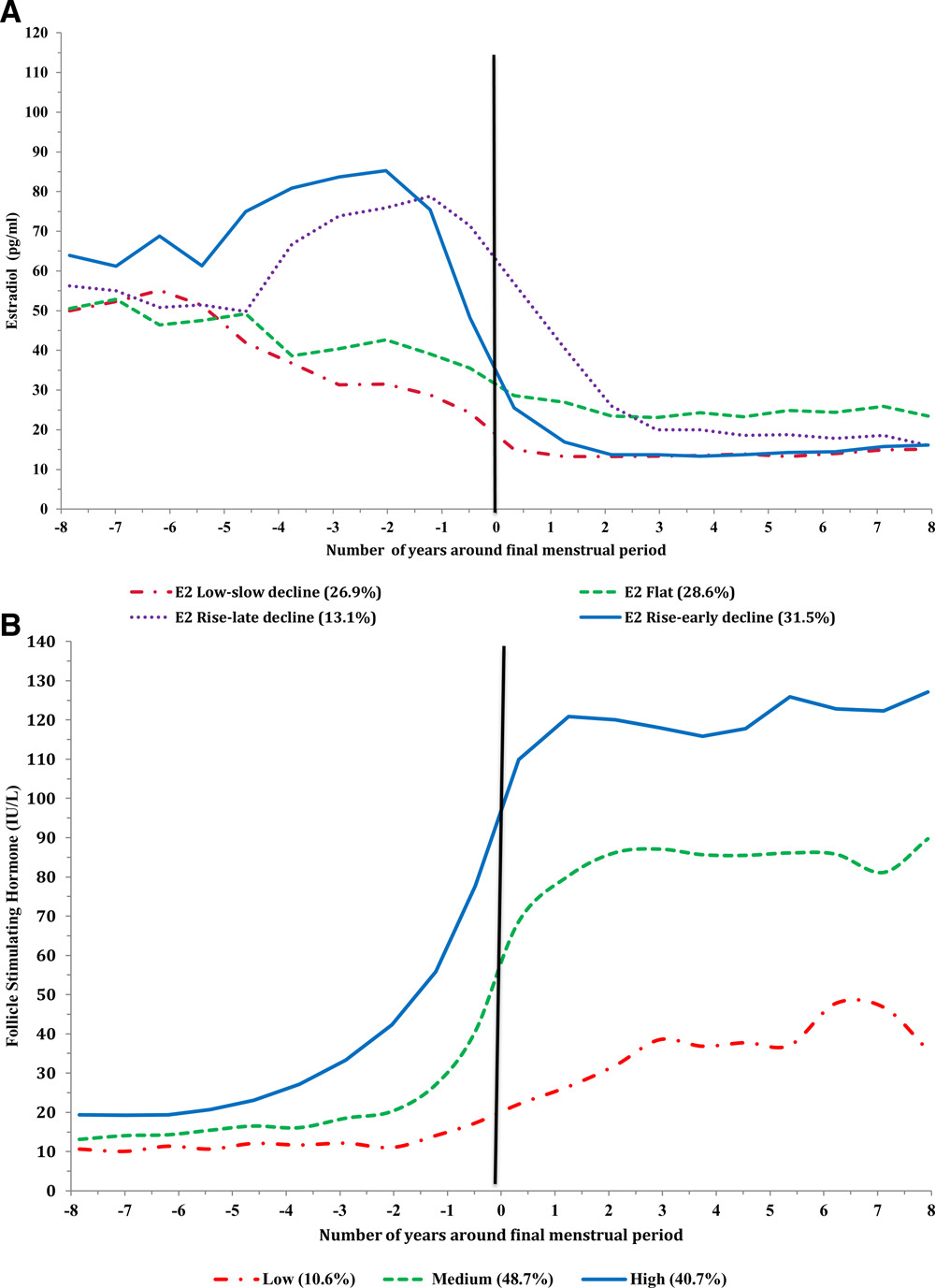
Remember -estradiol increases significantly 5.5 years before the FMP in 44.5% of midlife women, with a steep early decline almost 1 year before the FMP (estradiol rise–early decline) or a late estradiol decline after the FMP (estradiol rise–late decline). Two other common patterns of estradiol decline that are experienced by 55.5% of midlife women: a slow-decline or a flat pattern. During perimenopause there is no evidence of estradiol leaving the building, deficiency, flat lining, or dropping off a cliff - until the last 2 years before fmp, but then only a subsection of people.
So, when someone says boldly that you can still be having regular periods during perimenopause - that is wrong, based on STRAW.
When a GP (allegedly) asks if periods are still present and says, 'you can't be in perimenopause if you are still having periods' - that is also wrong.
When someone says 'perimenopause starts 7 to 10 years before periods stop' - that is likely to be wrong, unless the individual does indeed have periods changing in length in 7 days as early as 7-10 years before menopause day - which is very unlikely based on what we know about ovarian aging.
If someone says, 'signs and indicators, such as sadness, low mood, changes in sleep pattern, energy and generally feeling not yourself, is probably closely related to changes in ovarian activity, long before noticeable menstrual cycle changes happen.' - that is fair and accurate, and with a carefully designed question + answer system further insights could be collected and appropriate support offered🤔
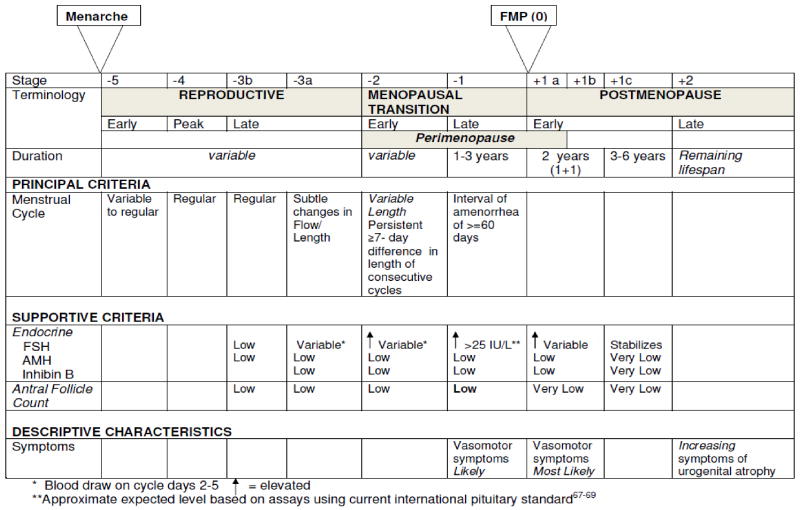
You can download the original STRAW staging system here https://pmc.ncbi.nlm.nih.gov/articles/PMC3340903/